A PATIENT wrongly diagnosed with arthritis and treated for more than 13 years with drugs he did not need has called for compensation from the government.
The man – whose name the JEP has agreed not to publish – is one of 340 rheumatology patients whose cases were recently reviewed, revealing what Health Minister Karen Wilson called ‘systemic governance problems’ in Health and Community Services.
The man told the JEP that when he had finished processing the situation, he believed it was right ‘to have a conversation with someone about compensation’.
Describing the impact of the arthritis diagnosis on his life, the man highlighted having to reduce working hours with a corresponding drop in salary; the effect on his wife and family; the unknown effects of unnecessary treatment; and the additional stress during the Covid pandemic of being designated a ‘high risk’ patient.
He said: ‘If somebody or a system has allowed something to go wrong, I don’t want my condition to define me, but there is a need to know exactly what’s going on. To be told it’s wrong, we think it’s fibromyalgia, but we’re discharging you anyway, doesn’t feel enough.’
The man was first referred to the Hospital’s rheumatology department in 2009 when he was diagnosed with seronegative arthritis – a form of the condition which does not display typical antibodies associated with the condition, making diagnosis more difficult.
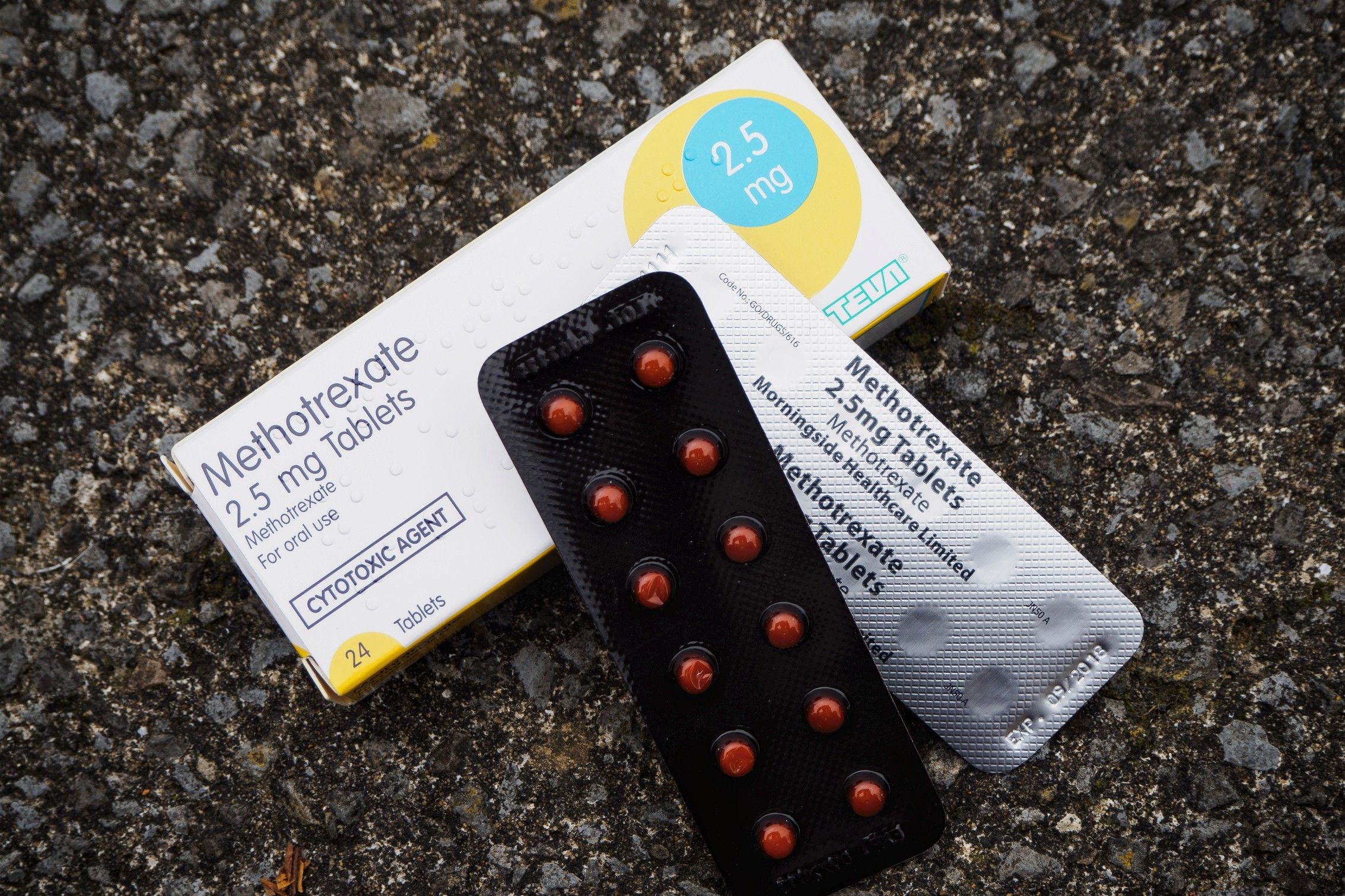
In the years that followed, he was prescribed a range of treatment from anti-inflammatory drugs to methotrexate – a chemotherapy agent and immune-system suppressant – and steroids, before receiving a weekly injection of biologic agents, naturally occurring substances used to treat rheumatic conditions.
He said he thought he was ‘lucky’ to be put on such treatment until he saw a specialist in rheumatology at the Hospital last year who cast doubt on the previous diagnosis. Posts on social media suggested his case was not an isolated one.
‘That doctor did something when I met him that the other doctors hadn’t done in the last 14 years. It sounds really crazy but he examined me. I said to him you are the first person who has actually asked me where my pain is and examined my body in those areas. At no point had those doctors done a physical examination – I’ve had scans and numerous blood tests but no doctor has ever physically examined me,’ he said.
This month, following an audit of rheumatology patients, the government admitted weaknesses in the service, including poorly written patient notes, some inappropriate prescribing, and prescriptions that did not include the clinical condition being treated. Announcing the conclusions, Deputy Wilson said that nobody should be in any doubt about the seriousness of the review and its findings.
Describing his meeting with one of the UK-based consultants who carried out the review, the patient, who approached the JEP, said: ‘She openly said to me that unfortunately she didn’t feel that I was struggling with seronegative arthritis and that actually I’d been misdiagnosed right back in 2009, and she openly apologised for that, which I thought was quite a statement. We talked about the medication I’d taken for all those years and again she apologised very clearly for that. I asked for a letter clarifying exactly what I was living with.’
The letter he received did not repeat the apology he said he had received in person, but it did confirm a diagnosis of fibromyalgia and some osteoarthritis, often known by doctors as ‘wear and tear’.
‘All I know is that I saw a consultant four weeks ago who told me I was wrongly diagnosed, wrongly prescribed and then promptly discharged me from the clinic but the chronology the consultant who was carrying out the review had was still wrong because she had talked about me being referred to rheumatology in 2015, whereas I was diagnosed back in 2009,’ he said.
The man continued: ‘It’s a huge frustration that so much time has been wasted and if you are taking injections that are inhibiting the way your body is working in certain situations. What does that do if your body didn’t need it? I don’t know and I need someone to tell me.
‘As the pain and that fatigue has changed and increased, I see the impact on my wife, who worries about me and sometimes is almost my carer at times. That really annoys me and I just want us both to be able to enjoy the next few years, whatever they bring. I don’t want to be worrying about my health.
‘Even thinking back to Covid and lockdowns, by the nature of my diagnosis and the medication I was taking, I was classified as a high-risk patient, so I removed myself from the office earlier and from social events. Because I was shielding for longer, I missed out on more than perhaps I needed to, and [there was] the worry for my children and family.’
He added: ‘I’m interested in having a conversation with someone who can give me an answer to find the best way to support me and my family going forwards, and some answers perhaps about how this happened, so that other people don’t find themselves in the same situation. I truly hope that this review recrystallises the Island’s focus on rheumatology. We needed more expertise than we had.’
Response from HCS
Responding to questions about compensation, HCS medical director Patrick Armstrong said it was too soon so draw any conclusions on any potential misdiagnosis until the Royal College of Physicians’ final report was published.
‘It is expected in the next few months and, subject to any legal constraints, we will be publishing [its] findings,’ he said.
Mr Armstrong added: ‘I would like to ask that any patients with concerns about their treatment arising from this matter, contact the HCS Patient Advice and Liaison Service by email on pals@health.gov.je or by telephone on 443515.’